Switch to Sciatica Treatment in Arlington, VA
What is Sciatica?
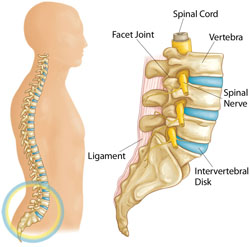
If you suddenly start feeling pain in your lower back or hip that radiates to the back of your thigh and into your leg, you may have a protruding (herniated) disc in your spinal column that is pressing on the roots of the sciatic nerve. This condition is known as sciatica.
Symptoms of Sciatica
Sciatica may feel like a bad leg cramp that lasts for weeks before it goes away. You may have pain, especially when you sit, sneeze, or cough. You may also have weakness, “pins and needles” numbness, or a burning or tingling sensation down your leg.
Causes of Sciatica
You are most likely to get sciatica between the ages of 30 and 50 years. It may happen as a result of the general wear and tear of aging, plus any sudden pressure on the discs that cushion the bones (vertebrae) of your lower spine. The gel-like center (nucleus) of a disc may protrude into or through the disc’s outer lining. This herniated disc may press directly on the nerve roots that become the sciatic nerve. Nerve roots may also get inflamed and irritated by chemicals from the disc’s nucleus.
Approximately 1 in every 50 people will experience a herniated disc at some point in their life. Of these, 10% to 25% have symptoms that last more than 6 weeks. In rare cases, a herniated disc may press on nerves that cause you to lose control of your bladder or bowel. If this happens, you may also have numbness or tingling in your groin or genital area. This is an emergency situation that requires surgery. Phone your doctor immediately.
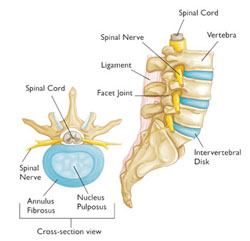
Normal lumbar anatomy/cross-section
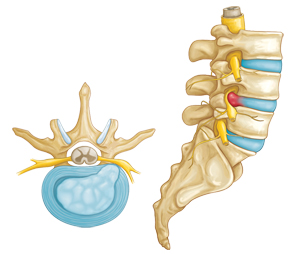
Herniated disc (side view and cross-section)
Diagnosis
Diagnosis begins with a complete patient history. Your doctor will ask you to explain how your pain started, where it travels, and exactly what it feels like. A physical examination may help pinpoint the irritated nerve root. Your doctor may ask you to squat and rise, walk on your heels and toes, or perform a straight-leg raising test or other tests. Most patients with sciatica have compression of the L5 or S1 nerve roots. X-rays and other specialized imaging tools such as magnetic resonance imaging (MRI) may confirm your doctor’s diagnosis of which nerve roots are affected.
Sciatica Treatment Options
Nonsurgical Treatment
The condition usually heals itself, given sufficient time and rest. Approximately 80% to 90% of patients with sciatica get better over time without surgery. Nonsurgical treatment is aimed at helping you manage your pain without long-term use of medications. First, you’ll probably need at least a few days of bed rest while the inflammation goes away. Nonsteroidal anti-inflammatory drugs such as ibuprofen, aspirin, or muscle relaxants may also help. In addition, you may find it soothing to put gentle heat or cold on your painful muscles.
Find positions that are comfortable, but be as active as possible. Motion helps to reduce inflammation. Most of the time, your condition will get better within a few weeks. Sometimes, your doctor may inject your spine area with a cortisone-like drug. As soon as possible, start physical therapy with stretching exercises so you can resume your physical activities without sciatica pain. To start, your doctor may want you to take short walks.
Surgical Treatment
You might need surgery if you still have disabling leg pain after 3 months or more of nonsurgical treatment. A part of the herniated disc may be removed to stop it from pressing on your nerve. The surgery (laminotomy with discectomy) may be done under local, spinal, or general anesthesia. You have a 90% chance of successful surgery if most of the pain is in your leg.
Rehabilitation
Avoid driving, excessive sitting, lifting, or bending forward for at least a month after surgery. Your doctor may give you exercises to strengthen your back. Following treatment for sciatica, you will probably be able to resume your normal lifestyle and keep your pain under control. However, it’s always possible for your disc to rupture again. This happens to about 5% of people with sciatica.
Testimonials for Dr. Ira D. Fisch, Back and Sciatica Specialist at OrthoBethesda in Maryland
Excellent orthopedic doctor and surgeon. I’ve seen Dr. Fisch over the years for various arthritis, sciatica, and spinal lumbar and cervical issues including epidural injections and spinal surgery. He’s excellent and I highly recommend him for Spinal orthopedic related issues. I put my full trust in him. He’s knowledgeable and offers practical advice and considers surgery as a last remedy. Aside from his great sense of humor, he’s a guy you can talk to. – J.G.
Schedule a Sciatica Appointment in Bethesda, MD, Today
Lower back pain might be resolved via physical therapy. However, if it persists, it’s time to schedule an appointment for sciatic nerve issues with OrthoBethesda in Bethesda, MD. The sciatic nerve deserves proper treatment and care from a trusted team of orthopedic doctors and surgeons. Our centers can provide medical advice and help with muscle pain through individualized care so that your weakness turns into strength. Call our center today for more information about dealing with pain at (301) 530-1010 or to schedule a consultation regarding your conditions. Your health is impacted by pain of all kinds, which is why we offer spinal stenosis as a treatment method for the low back region.
Further Reading
What Causes Sciatica Nerve Pain?
Spinal Decompression Therapy — How It’s So Effective
 ">
">
Call OrthoBethesda for Sciatica Treatment Today
If you are diagnosed with sciatica, you may require quality orthopedic treatment to alleviate your pain. Contact OrthoBethesda to make an appointment or call us at (301) 530-1010 today!