Switch to Neck Pain Treatment in Arlington, VA
Neck Pain
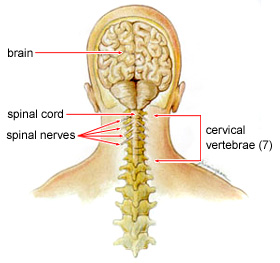
The neck (cervical spine) is composed of vertebrae that begin in the upper torso and end at the base of the skull. The bony vertebrae along with the ligaments (which are comparable to thick rubber bands) provide stability to the spine. The muscles allow for support and motion. The neck has a significant amount of motion and supports the weight of the head. However, because it is less protected than the rest of the spine, the neck can be vulnerable to injury and disorders that produce pain and restrict motion. For many people, neck pain is a temporary condition that disappears with time. Others need medical diagnosis and treatment to relieve their symptoms.
Cause
Neck pain may result from abnormalities in the soft tissues—the muscles, ligaments, and nerves—as well as in bones and joints of the spine. The most common causes of neck pain are soft-tissue abnormalities due to injury or prolonged wear and tear. In rare instances, infection or tumors may cause neck pain. In some people, neck problems may be the source of pain in the upper back, shoulders, or arms.
Inflammatory Diseases
Rheumatoid arthritis can destroy joints in the neck and cause severe stiffness and pain. Rheumatoid arthritis typically occurs in the upper neck area.
Cervical Disk Degeneration (Spondylosis)
The disk acts as a shock absorber between the bones in the neck. In cervical disk degeneration (which typically occurs in people age 40 years and older), the normal gelatin-like center of the disk degenerates and the space between the vertebrae narrows. As the disk space narrows, added stress is applied to the joints of the spine causing further wear and degenerative disease. The cervical disk may also protrude and put pressure on the spinal cord or nerve roots when the rim of the disk weakens. This is known as a herniated cervical disk.
Injury
Because the neck is so flexible and because it supports the head, it is extremely vulnerable to injury. Motor vehicle or diving accidents, contact sports, and falls may result in neck injury. The regular use of safety belts in motor vehicles can help to prevent or minimize neck injury. A “rear end” automobile collision may result in hyperextension, a backward motion of the neck beyond normal limits, or hyperflexion, a forward motion of the neck beyond normal limits. The most common neck injuries involve the soft tissues: the muscles and ligaments. Severe neck injuries with a fracture or dislocation of the neck may damage the spinal cord and cause paralysis.
Other Causes
Less common causes of neck pain include tumors, infections, or congenital abnormalities of the vertebrae.
When Should You Seek Medical Care?
If severe neck pain occurs following an injury (motor vehicle accident, diving accident, or fall), a trained professional, such as a paramedic, should immobilize the patient to avoid the risk of further injury and possible paralysis. Medical care should be sought immediately.
Immediate medical care should also be sought when an injury causes pain in the neck that radiates down the arms and legs.
Radiating pain or numbness in your arms or legs causing weakness in the arms or legs without significant neck pain should also be evaluated.
If there has not been an injury, you should seek medical care when neck pain is:
- continuous and persistent
- severe
- accompanied by pain that radiates down the arms or legs
- accompanied by headaches, numbness, tingling, or weakness
Many patients seek orthopaedic care for neck pain because orthopaedists are specifically trained to diagnose, treat, and help prevent problems involving the muscles, bones, joints, ligaments, and tendons. Although some orthopaedists confine their practices to specific areas of the musculoskeletal system, most treat a wide variety of diseases, injuries, and other conditions, including neck pain.
Further Reading
Spine Surgery: When It Works and When It Doesn’t
Spinal Decompression Therapy — How It’s So Effective
 ">
">
Contact OrthoBethesda to Treat Your Neck Pain
There are many factors that go into neck pain, that’s why it’s important to see a qualified orthopedic specialist to diagnose and offer the right treatment plan for you. Get in contact with one of our orthopedic specialists or call us at (301) 530-1010 to make an appointment today!