
According to statistics from the American Chiropractic Association, up to 80% of adults will experience back pain at some point in their life. That back pain accounts for more than 264 million missed workdays a year and is the third most common reason for doctor visits. Our backs are a complicated system of bones, ligaments, joints and muscles — with the spine at the center of it all. When you have back pain, pinpointing the issue and choosing a treatment path requires careful consideration.
If you’re experiencing back pain that stems from your spine, you want to find answers that allow you to return to normal life. After failed non-surgical attempts at recovery, you may consider spine surgery. Back surgery is an ideal solution for some people, but it may not be the right fit for everyone. The following is helpful information to consider when deciding if back surgery could be for you.
Is Spinal Surgery Dangerous?
The answer to the question, “Is lower back surgery dangerous?” is both yes and no. Every surgical procedure has risks, including spinal surgery. The nature of spinal surgery increases the risk of severe complications compared to other procedures. Spinal surgery happens at and around sensitive areas in the spine and spinal cord. The most significant risks you could face if an error occurs during surgery include paralysis or a spinal infection.
Despite the possibility of severe complications, the mortality rate for spinal surgeries is low. One study found a mortality rate of 0.13% out of 803,949 lumbar spine surgery patients. The rate of surgical complications is also low, with a 7.6% complication rate in a study of 3,475 patients. Your back surgery may deviate from standard risk levels, depending on your existing health conditions and the type of surgery you’re having.
What Makes Spinal Surgery Dangerous?

Much of the potential danger in a spinal surgery links to the potential bodily risks if something goes wrong during the procedure. The spine and spinal cord play pivotal roles in bodily strength, sensation and movement. Mistakes or complications during surgery could impair one or more of these functions. In addition to these dangers, a more involved surgical procedure could present more significant risks than a simple procedure.
Aside from danger, one of the paramount concerns for back surgery is whether or not it is successful.
What Percentage of Back Surgeries Are Successful?
One study estimated the success rate for back surgeries to be about 50%. This estimate is conservative, as most success rates depend on a wide variety of factors. Your health, specific surgery, source of pain and any surgery complications influence whether or not your procedure will be effective.
What Percentage of Back Surgeries Fail?
The American Society of Anesthesiologists estimates that 20 to 40% of back surgeries fail. Patients having repeated back surgeries have a much higher chance of failure. One study found only 30% of second back surgeries are successful. The number decreases for third and fourth back surgeries, with a 15% and 5% success rate, respectively.
Unfortunately, failed back surgery is common enough that it has received classification as a medical condition. Failed back surgery syndrome (FBSS) occurs when a patient experiences continued pain in the back, neck or limbs following a surgery meant to reduce pain.
How Common Is Failed Back Surgery?
Failed back surgery is relatively common — but not because the surgeon performed the procedure incorrectly. Back surgery can only accomplish two goals: decompressing a pinched nerve root or stabilizing a painful joint. If a pinched nerve or painful joint is the source of a patient’s pain, a doctor may be able to address the issue with surgery.
However, it can be challenging to identify and diagnose one of these factors before surgery. One of the most common reasons back surgery doesn’t work is because the surgery selected does not address the source of a patient’s pain. Considering appropriate non-surgical measures before surgery can help you avoid a costly procedure that does not adequately address back pain.
What Are the Possible Complications After a Procedure of the Spine?
Though the complication rate for back surgeries is relatively low, there is still potential for a variety of health issues. The following are some common complications to consider.
- Deep venous thrombosis: Following a surgery near the pelvis or lower extremities, patients may experience blood clotting in the calf, thigh or pelvis. This phenomenon occurs as the body tries to stop bleeding following the surgery. It may also occur if blood vessels near the surgery site get injured.
- Dural tear: If surgery disrupts the protective covering over the spinal cord and nerves, you could have a dural tear. Surgeons may detect and repair a dural tear during surgery, and most tears heal without an issue. If the tear does not heal properly, you may experience headaches from leaking spinal fluid.
- Lung issues: If you undergo general anesthesia, you may experience temporary lung function issues following the surgery. Exercising your lungs before and after surgery is helpful to promote optimal function and recovery.
- Infection: Spinal surgeries have a low infection rate, but it is possible. If the incision site becomes infected, the infection can spread to the spinal cord and vertebrae. Many doctors will prescribe antibiotics before surgery to help prevent infection, especially if your surgery involves metal hardware or a bone graft.
- Hardware malfunction: Many spinal surgeries use screws, rods and plates to help vertebrae heal in proper alignment. If one of these hardware pieces breaks or moves before the bone has a chance to heal, you may need another surgery to correct it.
- Continued pain: If your surgery is not successful, you may feel continued pain after you’ve recovered. In worst-case scenarios, surgery may increase your pain. It’s essential to identify your pain source as accurately as possible before having surgery to decrease your chance for FBSS.
- Sexual dysfunction: The spinal cord and nerves transmit signals throughout your body. You may experience sexual dysfunction if surgery damages the nerves near your pelvic region.
- Transitional syndrome: In a healthy spine, all the vertebrae work together to distribute the load from your body. After back surgery, vertebrae adjacent to the problematic ones may take on an uneven load while the spine heals. This issue could accelerate wear in the nearby vertebrae and cause pain.
- Pseuodoarthrosis: If you undergo a spinal fusion surgery and your vertebrae do not successfully fuse, you may have continued pain from pseudoarthrosis. You may require additional surgery to fix this condition if it does not heal or worsens over time.
You may be less likely to experience specific complications based on your health condition. Talk to your doctor to learn about a list of complications that could be pertinent to you following a spinal surgery.
Spinal Surgery Success Rates
As mentioned before, several factors impact spinal surgery success rates. Your surgery method, the condition you’re attempting to fix, your surgeon, aftercare plan and more play into the results you may experience. For example, your low back surgery success rate may vary, depending on whether your low back pain stems from a pinched nerve or herniated disc.
Though the percentages given in this section indicate general success rates, you’ll need to talk to your surgeon to determine a projected success rate for your unique situation.
Thoracic Spine Surgery Success Rate

The thoracic spine is in the middle of the spine, between the abdomen and upper back. You may have thoracic spine surgery if you’ve severely herniated a thoracic disc or if you have one of the following conditions:
- A compression fracture
- Degenerative disc disease
- Kyphosis
- Scoliosis
- Spondylolisthesis
According to one study, patients who had thoracic spine surgeries with the posterolateral approach had a complication rate of 12 to 30%. After 17 months of recovery, 76.9% of these patients reported satisfaction with the success of their surgery.
Minimally Invasive Spine Surgery Success Rate
A surgeon might use minimally invasive spine surgery (MIS) to stabilize vertebrae and spinal joints or relieve pressure on spinal nerves. This approach is a more conservative method compared to other open spine surgeries. Surgeons use small incisions, microscopic video cameras and guiding instruments to minimize the amount of trauma to the surgery site.
You may qualify for MIS if you have one of the following conditions:
- Degenerative disc disease
- Compression fractures
- A herniated disc
- Lumbar spinal stenosis
- Scoliosis
- Spinal infections
- A spinal tumor
- Spondylolisthesis
There are several types of MIS procedures, depending on where a surgeon makes their incision. For an MIS transforaminal lumbar interbody fusion, success rates range from 60 to 70%, with an 80% satisfaction rate for patients. For an MIS posterior lumbar interbody fusion procedure, patients experienced a 90 to 95% successful fusion rate.
Herniated Disc Surgery Success Rate
Herniated discs are common in the lumbar spine, but they may also occur in the cervical spine near the neck. If your discs have degenerated with time and ruptured, you may require herniated disc surgery. Depending on the location of your herniated disc, you may require a different surgical procedure.
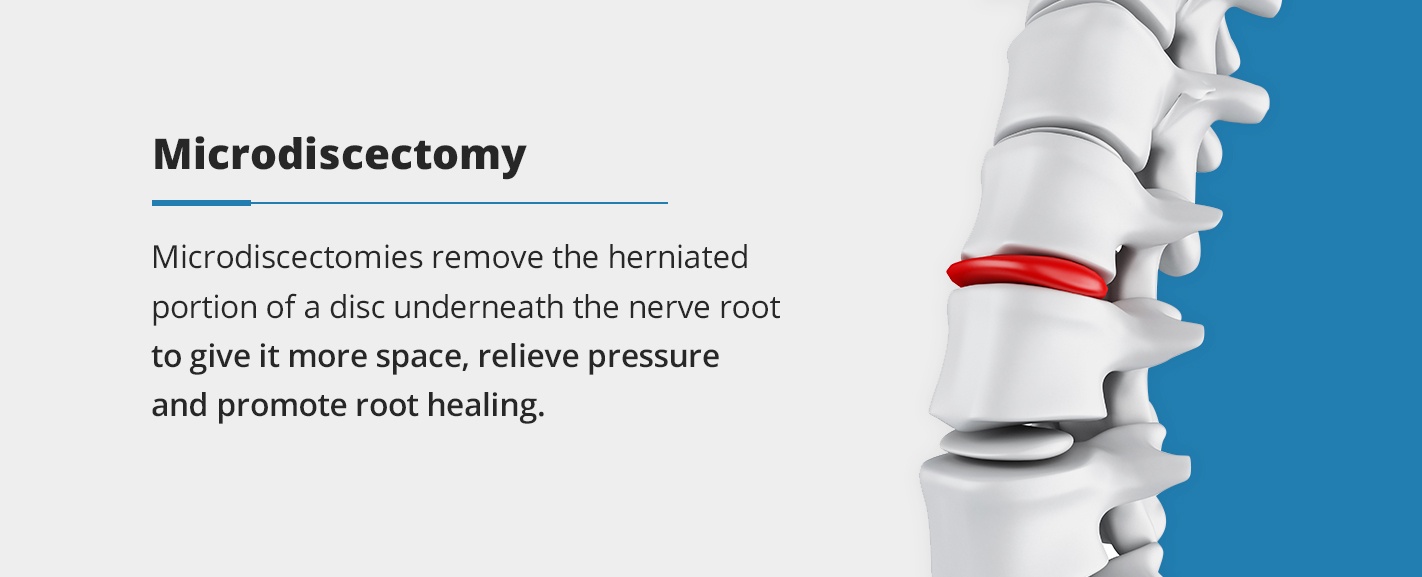
- Microdiscectomy: This procedure is common for herniated lumbar discs. Microdiscectomies remove the herniated portion of a disc underneath the nerve root to give it more space, relieve pressure and promote root healing.
- Discectomy: A discectomy is common for herniated cervical discs. Surgeons remove disc material through the front or back of the neck and fuse the disc space to take pressure off the spinal cord and nerve roots.
According to one study, the success rate for a herniated lumbar disc surgery was 78.9% among 39,048 patients. This same study reported a 94% long-term success rate for patients undergoing herniated cervical disc surgery.
Spinal Fusion Surgery Success Rate
Several spinal fusion surgeries can help limit back pain that stems from specific points. A fusion surgery involves joining two vertebrae with a bone graft, so they become one solid bone. This procedure can give your spine more stability and address pain you may feel when moving.
You may consider a spinal fusion surgery if you have one of the following conditions:
- Numbness, weakness or tingling in your legs
- Pain in your buttocks, back, thighs or legs
- Kyphosis
- Scoliosis
- Vertebrae injuries
- Spinal tumors or infections
Depending on the condition the surgery is treating, spinal fusion has a 70 to 90% success rate.
Sciatica Surgery Success Rate

Sciatica occurs when you feel sudden pain in your hip and lower back that radiates to the back of the leg and thigh. You may experience sciatica as a result of normal wear and tear that accompanies aging. About 80 to 90% of individuals with sciatica will experience relief without the need for surgery. However, sciatica surgery may be appropriate if you feel disabling leg pain even after non-surgical intervention.
If most of your sciatica pain is in your legs, there is a 90% surgery success rate with a laminotomy and discectomy.
Why Do So Many Back Surgeries Fail?
If most back surgeries have a greater than 50% average success rate, why is FBBS an issue? The answer is that most back surgeries rely on a variety of factors for success. These include patient health, the type of spine surgery a patient has and the way post-operative factors play out.
Patient Factors
Your health may influence the rate and success at which you recover. According to one study, the following conditions could negatively affect back surgery success:
- Preexisting patient depression
- Poor psychosocial well-being
- Smoking
- Obesity
- Patient age
- Hypertension
Spine Surgery Factors
If the surgical method used is not appropriate to address a patient’s pain, they will likely have a higher risk of back surgery failure. If there are any errors or complications during the operation, the surgery may have a greater risk of failure as well.
Post-Operative Factors
Back surgeries may not be as successful if a patient has one of the following conditions soon after surgery:
- A hematoma in the epidural or subdural areas
- Spinal infection
- Collection of fluid near the spine
- A nerve injury
Surgery may also have decreased effectiveness if a patient experiences transition syndrome as they recover.
Is It Worth It to Have Back Surgery?
Before you consider back surgery, doctors typically recommend you try conservative, non-surgical options. Most physicians suggest a three-month time window for these options, as many back issues will resolve themselves after that time. If you’ve completed non-surgical intervention and still struggle with back pain, you may want to talk to your doctor about surgery.
The National Institute of Arthritis and Musculoskeletal and Skin Diseases recommends surgery in the following situations:
- When a patient has a ruptured or herniated disc and damage to one or more discs
- When a patient has degenerative disc disease due to aging
- When a patient has spinal stenosis that narrows the spinal column and puts pressure on the spinal cord and nerves
- When a patient has spinal fractures attributed to osteoporosis
- When a patient has spondylolisthesis and one or more bones slips out of place
Whether you fall into one of the above categories or not, there are several crucial questions to consider before pursuing surgery:
- What are the surgery risks, and how could they affect me?
- What are the potential long-term consequences if I have back surgery?
- What are the potential long-term consequences if I don’t have surgery?
- What is the recovery time for the procedure?
- What does recovery entail?
- How long will I be unable to work?
- How experienced is the surgeon?
- What are the physician and surgeon recommendations for the procedure?
- What is the success rate for this type of surgery for my specific pain?
Different Options for Spine Treatment
No matter your situation, treatment options range from general to specific. Talk to your doctor to determine what may be appropriate for your back pain.
Non-Surgical Options for Back Pain

Before having back surgery, non-surgical treatments like the following can help mitigate or completely relieve your pain.
- Heat and ice: Alternating between a heating pad and cold pack may be enough to relieve temporary back pain.
- Pain medication: You may be able to address back pain with over-the-counter acetaminophen, or your doctor may prescribe a stronger drug. Each pain medication has trade-offs in strength versus long-term consequences, which you should discuss with your doctor.
- Epidural steroid injections: If heat, ice and pain medications do not address your pain, your doctor may recommend an epidural steroid shot. These injections, administered to the spine, can help decrease inflammation in the affected area.
- TENS units: A TENS unit has sticky electrode pads that connect to a small, battery-operated device. You can position the electrodes over the painful area, and the device will deliver an electric current. This stimulation masks and reduces the pain you feel in the affected area.
- Lifestyle changes: You may be able to address your back pain by changing some of your habits. If so, your doctor may recommend losing weight, quitting smoking, improving your posture or modifying your activities.
- Physical therapy: If your back pain lasts from two to six weeks, your doctor may recommend physical therapy. Your physical therapist may guide you through stretches and strengthening exercises to help with your pain.
Surgical Methods
If you still feel severe pain after three months of non-surgical intervention, you may want to consider surgery. Depending on where you’re experiencing pain and what is causing that pain, there are several surgical methods available.
- Artificial disc replacement: If one of your vertebral discs has become severely damaged, your doctor may recommend an artificial disc replacement procedure. This method partially or wholly replaces your damaged disc to help reduce pain and mitigate your risk for future disc degeneration.
- Discectomy: A discectomy removes a herniated disc that puts pressure on your nerve root or spinal cord. Your doctor may recommend having both a discectomy and a laminectomy performed at the same time.
- Laminectomy: A laminectomy removes bone spurs and the bony walls of painful vertebrae to open the spinal column and relieve pressure on your spinal nerves. This procedure may relieve pain, weakness or numbness from spinal stenosis.
- Foraminotomy: In a foraminotomy, a surgeon enlarges the bony hole through which the nerve root exits. This technique helps prevent bulging disks or thickened joints from pressing on the nerve.
- Fusion: A spinal fusion procedure removes a damaged disc between two vertebrae, then fuses those vertebrae with a bone graft or metal hardware.
- Vertebroplasty and kyphoplasty: Your doctor may recommend these procedures if you have a compression fracture from osteoporosis. In a vertebroplasty and kyphoplasty, surgeons use a bone cement material to harden and strengthen bones.
Pursue Back Pain Solutions at OrthoBethesda
If you’re struggling with back pain and you’re not sure what to do next, talk to the experts at OrthoBethesda. We have committed to taking a conservative approach for treating back and spinal issues, and we can guide you through a safe and effective treatment progression.
Our physical therapists will work with you to establish a physical therapy or injection plan before you consider surgery. If surgery is the best option after non-surgical treatment, our skilled surgeons will meticulously choose and carry out an effective surgery plan. For more information about how you can find relief, contact us today.
Related Content
- How to Prevent Back Pain When Working From Home
- How to Reduce Low Back Pain
- How to Sleep After Back Surgery
- 10 Steps to Achieving Better Posture
- How to Sleep With a Herniated Disc
- How to Know if You Have a Herniated Disc
- Spinal Fusion Surgery – Commonly Asked Questions
- Dr. Eric Feuchtbaum Makes Advancements in Minimally Invasive Spine Surgery With Mazor Robotics
- What Is Kyphosis?
- What Causes Sciatica Nerve Pain?
- Everything to Know About Scoliosis

