
Quick Navigation
- The Anatomy of the Shoulder
- Causes and Symptoms of Rotator Cuff Problems
- Detailed Guide to Shoulder Surgery Recovery
- Things You Need After/Post Shoulder Surgery
- Recovery Room and Getting Home
- At-Home Care
- Ice Compression
- Medication
- Surgical Incision Care
- How to Dress After Shoulder Surgery
- Signs of Complications
- Sleeping After Shoulder Surgery
- Driving After Surgery
- How to Recover From Shoulder Surgery Faster
- Contact OrthoBethesda
The speed and pain involved in recovering from shoulder surgery depend upon many factors, including the type of surgical procedure you had, absence or presence of complications, adherence to physician instructions, consistency in performing rehabilitation and physical therapy exercises and more. But whether you have a minimally invasive rotator cuff surgery or a total shoulder replacement, recovery from shoulder surgery takes time.
Below are some shoulder surgery recovery tips to help make your recovery as fast as possible. First, it’s helpful to learn about the anatomy of your shoulder and causes of common problems, such as rotator cuff issues.
The Anatomy of the Shoulder
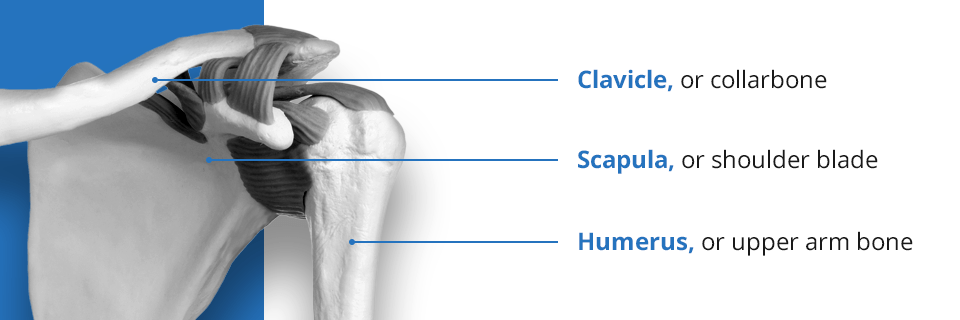
The shoulder is a complex joint capable of more movement than other joints in the body. It’s made up of several bones.
- Clavicle, or collarbone
- Humerus, or upper arm bone
- Scapula, or shoulder blade
Besides bones, other components are responsible for function and movement.
- Ball and socket: Your upper arm bone head fits into your shoulder blade through a rounded socket known as your glenoid. Your articular cartilage, which is a slippery tissue, covers the surface of your ball and socket, creating a frictionless, smooth surface that helps your bones easily glide across one another. Strong fibrous cartilage rings your glenoid, which creates a gasket around your socket, adding stability and cushioning the joint.
- Shoulder capsule: Bands of tissue called ligaments surround your joint, forming a capsule that holds it together. Your synovium, which is a thin membrane, lines the capsule’s undersurface. It makes synovial fluid that provides lubrication for your shoulder joint.
- Rotator cuff: You have four tendons surrounding your shoulder capsule that help center your arm bone in your shoulder socket. This is your rotator cuff and is a thick tendon material. Your rotator cuff covers your humerus head, attaching it to your shoulder blade.
- Bursa: Your bursa is a lubricating sac between the bone on top of the shoulder and your rotator cuff. Your bursa helps your rotator cuff tendons smoothly glide when you’re moving your arm.
Causes and Symptoms of Rotator Cuff Problems

Sometimes, your rotator cuff tendons can become pinched by the surrounding bones or can tear. Issues like these can happen due to an injury such as falling on your arm. However, wear and tear over time can do a number on your shoulder as well, causing severe pain.
Common symptoms of rotator cuff problems are:
- Weakness
- Loss of motion
- Stiffness
- Trouble raising your arm overhead
- Pain occurring mainly at night
- Cracking sensation when you move your shoulder
You can treat many rotator cuff problems at home. Your doctor might suggest shoulder arthroscopy if you have a condition that’s painful and doesn’t respond to nonsurgical treatment. While you need to know how to prepare for shoulder surgery, you also need to know proper postoperative recovery tips.
These rotator cuff surgery recovery tips could help make the healing process better, allowing you to start participating again in physical activities.
Detailed Guide to Shoulder Surgery Recovery
Here, you’ll learn what to expect after arthroscopic shoulder surgery so you can properly plan for your operation and manage your recovery better.
Things You Need After/Post Shoulder Surgery
To help make your recovery a smoother process, consider buying the items below before going in for your shoulder surgery.
- Detachable showerhead: You’ll likely need to keep your incision dry for a certain period. Detachable shower heads make it simpler to avoid wetting your incision.
- Shower chair: A shower chair will help minimize your risk of falling since you can sit down while you shower. These are helpful after you’ve had surgery or if you’re taking pain medications which can make you dizzy or tired.
- Waterproof bandages or plastic bags and athletic tape: You may want to cover your incision with a large waterproof bandage or plastic bag using tape to keep it from getting wet until your doctor says it’s OK to do so.
- Pump soap: Use soap from a pump container to make showering simpler with one arm.
Recovery Room and Getting Home

Following your surgery, you’ll remain in the recovery room for an hour or two before the doctor discharges you. Nurses will provide you with pain medicine, if necessary, and monitor your responsiveness. You’ll need to have another person drive you home, because you’ll be wearing a sling around your arm and could still be feeling the effects of the general anesthetic, which will make driving dangerous.
The person driving you home or another person should stay with you for the first night at least and help make you feel more comfortable, prepare your meals and help with other things. You may want to have them check up on you daily for the first week home to help with daily tasks and see if you need anything. Having someone assist you will help you avoid shoulder pain and ensure you adhere to postoperative instructions and rehabilitation restrictions.
At-Home Care
While recovering from arthroscopic shoulder surgery is often quicker than recovering from open surgery, it could take several weeks for your shoulder joint to heal completely.
You should expect some discomfort and pain during the first week following surgery — maybe even longer. But, if your surgery was more extensive, it could take a few weeks before the pain goes away.
Ice Compression
Use a cold pack to reduce inflammation and pain. You can use a bag of peas wrapped in a light cloth, or you can buy an ice pack and place it directly on your shoulder for about 20 minutes every few hours for your first three to five days.
Once you’ve gotten past this phase, you can use a heat pack or other heat device which can be soothing.
Medication

Your doctor may prescribe you pain medicine if the pain is hard to tolerate. You might experience bruising, stiffness and swelling of your hand and arm, in addition to pain. These are normal symptoms and stem from the shoulder healing process.
Many types of pain medicine are available to reduce swelling and control your pain.
- Local anesthetics: These numb the painful area.
- Opioids: Only take these powerful drugs short-term, since they are highly addictive.
- Nonsteroidal anti-inflammatory drugs: These include Advil or ibuprofen.
Treating the pain with medicine can make you feel more comfortable, which will help your shoulder surgery recovery go more smoothly.
It’s essential to always use opioids exactly as prescribed, since they can be habit-forming. Once your pain starts improving, you should stop taking the opioids. If you still require pain medication, switch to other types of pain relief.
Surgical Incision Care
Change your dressing as the doctor instructs until they remove your stitches. Typically, this occurs a week following surgery. After your doctor removes your stitches, they might allow you to rinse the wound. Don’t soak the incision site in a bath or take long showers. Make sure you dry the wound thoroughly after your shower.
How to Dress After Shoulder Surgery
In the early phase of your recovery, you should wear loose-fitting clothing you can easily put on and that fit over your sling. Wear shirts with a zipper or easy-to-use buttons, rather than having to pull them over your head. Shirts that don’t require you putting your arm above shoulder level will be best.
Wear bras that close in the front to make them easier to put on during your early post-operative phase. If you don’t have or can’t purchase a bra like this, put the bra on backward where the clasp is in the front, and then twist it around to your back once clasped.
Wear shoes you can put on easily with one hand, preferably with no laces, since trying to tie shoelaces with a single hand could be a big challenge. Velcro or slip-on shoes are best.
Signs of Complications

Although rare, you could experience complications from your rotator cuff surgery, like nerve damage or infections. Your doctor will go over potential complications with you. Immediately let them know if you’re experiencing any of these symptoms:
- Yellow discharge or redness at the incision sites
- Fever of 101 degrees or higher
- Numbness or tingling in your fingers or hand on the affected side
- Severe and sudden pain or pain not responding to medication
Sleeping After Shoulder Surgery

It can be a challenge trying to find a comfortable sleep position after shoulder surgery. Here are some rotator cuff surgery recovery sleeping tips your doctor will likely have you follow:
- Sleep on the opposite side, since initially, you won’t be able to put pressure or weight directly on the affected shoulder. You can also use pillows for propping yourself up into a more upright position.
- Lie flat to sleep, as your pain and discomfort begin to decline.
- Add some pillows behind your back to help keep you from rolling back on the affected shoulder. You can also use wedge-shaped pillows, or you can stuff something underneath your mattress to make it tilt slightly, which will make it harder for you to turn over.
- Switch sides with your partner to help keep you sleeping on your unaffected shoulder, depending on your sleeping habits and the side you usually sleep on.
- If you live alone, try putting your bed up against a wall to keep you from turning toward the wall side.
- Elevate your shoulder by placing pillows under it. Doing this will help with swelling and keep you from turning onto your shoulder.
- Keep your affected arm in a sling to help keep your shoulder protected and prevent unnecessary movement.
Driving After Surgery
Prepare yourself for the fact that it will likely be up to six weeks before you can drive again. Having the use of only one arm to control the vehicle makes driving unsafe, especially in an emergency. With shoulder exercises and rehabilitation, most individuals can move their arms enough to start driving after around six weeks.
Given your range of movement restrictions following shoulder surgery, particularly if the surgeon reattached torn rotator cuff tendons, you will understand why you shouldn’t drive for the first six weeks. It will also hopefully make you motivated to start rehabilitation exercises right away to build up strength and endurance and range of movement.
If your shoulder procedure was minor, like a bursectomy or subacromial decompression, you might be able to start driving again at an earlier stage. That is because you would only need your sling for five to seven days, and after three to four weeks, you’d likely feel comfortable enough to start driving again. You’d need to talk with your doctor about this, since each case is different.
You should start by taking short drives when the roads aren’t busy to see how you do. Once you can handle this safely and properly, you can slowly increase the duration of your driving and begin driving in busier traffic.
How to Recover From Shoulder Surgery Faster

Here are some of the best shoulder surgery tips for quicker recovery.
1. Know the Stages of Rehabilitation After Shoulder Surgery
Your physical therapist will guide you through these rehabilitation stages.
- Immobilization: Uses a sling to stabilize your shoulder for several weeks as your joint heals.
- Passive exercise: Relies on assistance and support of your physical therapist or a specific machine to move your arm gently starting a few weeks after surgery.
- Active exercise: Moves your shoulder and arm by using your muscles beginning up to three months following your surgery.
As you continue progressing through rehabilitation, weightlifting exercises and gentle stretches can help you with your range of motion and gaining endurance. Performing some of these exercises in a pool eases the impact on your shoulder.
2. Don’t Resume Physical Activity Too Soon
Even if you’re not feeling a lot of pain, you still need to follow the doctor’s instructions about when you can do certain things during your recovery time. Attempting to perform challenging exercises, activities or sports that place a strain on your shoulder may cause another injury. You could even injure other parts of your body like your elbow or spine when resuming physical activities too soon.
When you reach the six-week anniversary of your surgery, your doctor will decide if you can resume physical activities and go back to work. If your routine involves intense movement or heavy strain, you might require extra physical therapy sessions.
3. Embrace Physical Therapy

A physical therapist will see you on the day of your surgery, typically a few hours after you arrive and then twice a day for the subsequent days. They’ll provide you with an exercise program to help increase your range of motion. They’ll also educate you on safety with gait and transfer training and joint positioning.
Ultimately, your participation and motivation with physical therapy are the most crucial elements in your long-range rehabilitation, as far as speed and success are concerned. Your therapist will go over your routine exercise program with you, so you know what you’ll need to do when you get home. You’ll want to follow the exercises they instruct carefully and don’t overexert your strength. If you become fatigued or sore, pause because your muscle needs time to adapt and recover.
4. Perform Shoulder Surgery Exercises

The doctor will probably instruct you to straighten and bend your elbow, perform gentle pendulum motions and clench and unclench your fist regularly to improve comfort and facilitate blood flow.
Here are some potential exercises you may be instructed to perform. Be sure to talk with your doctor or therapist before you begin any of these if they haven’t included them in your exercise program.
Isometric exercises are a safe way to begin working your rotator cuff muscles following shoulder surgery. Isometric means your shoulder muscles contract, but with no motion. You perform isometric exercises like this:
- Keeping your elbow at a 90-degree angle, stand along a wall sideways.
- Place the outside of your forearm against the wall.
- Press into the wall while you contract your muscles, without moving your shoulder.
- Hold for five seconds and then repeat another five times.
- Place the inside of your forearm against the wall, after turning 180 degrees.
- Perform steps two through five again.
Regular exercises for restoring flexibility and motion to your shoulder and returning slowly to your daily activities is essential for a full, successful recovery from shoulder surgery.
Your physical therapist and doctor might suggest you exercise for two or three 15-minute sessions a day during your period of recovery. They may recommend some of the below exercises or others for helping prevent stiffness in your hand and elbow.
- Shoulder forward elevation: You’ll either lie down or sit down for this exercise. Lifting your arms above your head, clasp your hands, making sure to keep your elbows very straight. Hold this elevation for about 20 seconds, then lower your arms slowly. As the days progress, gradually increase your arm elevation, backing off if you feel any pain. Perform three sessions a day, 10 to 20 times per session.
- Pendulum, circular: Bend forward 90 degrees at your waist and place the hand of your unaffected arm on a table for support. Rock your body in a circular motion 10 times to move your arm clockwise, then do it 10 times counterclockwise. Keep your arm relaxed while you’reperforming this exercise. The circular pendulum movement should happen through the joint of your shoulder. Perform three sessions daily.
- Neck flexion: With your chin tucked slightly and your head in a comfortable position, bring your left ear to your left shoulder gently and hold this position for five seconds. Now, repeat with the right side. Continue doing this five times. Perform three sessions daily.
- Flexion/extension: Sit or stand with one arm extended palm-up in front of you. Bend your elbow slowly while raising your forearm to your shoulder. Relax your arm and repeat this exercise five times. Perform three sessions daily.
- Walk-up exercise: Straightening your elbow, use your fingers to “crawl” up a doorframe or wall as far as you can. Hold for 20 seconds and then repeat five to 10 times each session. Perform three sessions daily.
- Supported shoulder rotation: Keeping your shoulder blades together and down and elbow in place, slide your forearm back and forth. You may also use a cane or stick with this exercise to assist your arm outward while you keep your elbow to your side. Repeat this exercise 10 times each session. Perform three sessions daily. Your doctor might restrict the degree of external rotation of your affected shoulder following surgery. Before you perform this exercise, be sure to check with your physical therapist or doctor to see if you’ll have a limit on the external rotation.
- Shoulder internal rotation: Use a towel or your other hand to help bring the hand of your affected arm behind your back, and then across to the other side. Repeat 10 times each session. Perform three sessions daily.
The doctor might modify your routine after your first follow-up appointment based on your progress.
5. Know Recovery Times Can Vary
Because people have different health conditions, full recovery time will be different for everybody.
You might not require a sling if you’ve had a minor repair, and your strength might come back after a short period of rehabilitation. In cases like these, you might be able to go back to work or school within a few days of your surgery.
More complicated procedures will take longer to recover. Complete recovery might take a few months with arthroscopic shoulder surgery. Although recovery can be a slow process, following your doctor’s instructions and your rehabilitation plan is crucial for a successful outcome.
Contact OrthoBethesda for Orthopedic Treatment for Your Shoulder Ailment or Injury
If you’re experiencing pain in your shoulder, it’s time to schedule an appointment at OrthoBethesda. Our doctors will determine the cause of your pain and develop a personalized treatment plan. At our patient-centric orthopedic care center, our entire staff has dedicated their skills to providing you with individualized care, from evaluation to diagnosis to treatment to recovery.
Related Content
- Can a Rotator Cuff Tear Heal Without Surgery?
- Can You Drive After a Rotator Cuff Repair?
- Complete vs. Partial Rotator Cuff Tears
- Rotator Cuff Disorders: The Facts
- The Difference Between Rotator Cuff Tears and Shoulder Tendonitis
- Types of Rotator Cuff Tears
- When Not to Have Rotator Cuff Surgery
- Shoulder Pain – Frozen Shoulder
- How to Avoid Shoulder Pain While Playing Golf
- Why Sleeping on Your Side Is Killing Your Shoulder
- Shoulder Pain – Cervical Spine
- Does a Broken Shoulder Need Surgery?
- How Dr. Craig Miller Uses New Technology to Improve Shoulder Surgery
- Shoulder Arthritis and Shoulder Replacement
- How to Sleep After Shoulder Surgery


